The Hidden Headache of Mental Health Documentation—and the AI Tool That’s Finally Fixing It
✍️ If you’re a mental health clinician, you already know this truth: your second job isn’t therapy—it’s paperwork.
Behind every meaningful session lies an hour (or more) of mental health documentation. There are SOAP notes to write, ICD codes to choose, and compliance rules to follow. None of this work is optional. Notes support quality care, protect your license, and make billing possible. But when documentation spills into evenings and weekends, it drains your time, focus, and energy. Over time, that drain can turn into burnout.
This article breaks down the problem, step by step, in plain language. It also explains how an AI assistant called SOAPsync reduces the strain without compromising your standards. Think of this as a detailed guide for clinicians who want less paperwork, better notes, and more time to do what actually matters—helping people.
Why Mental Health Documentation Matters (And Why It’s So Draining)
Mental health documentation is more than a record of what happened. It serves four major purposes:
- Legal protection and ethical accountability.
Your notes show what you observed, what decisions you made, and why. If there’s ever a complaint, audit, or legal issue, your documentation becomes your evidence. - Payment and reimbursement.
Insurers reimburse based on what you document. If the note is vague, incomplete, or coded incorrectly, claims get delayed or denied. That costs time and money. - Continuity of care.
Good notes help you remember details across sessions, guide long-term treatment, and coordinate with other providers when needed. - Clinical decision support.
Writing organized notes forces you to reflect: What changed? What worked? What should we try next? Documentation can make your thinking more precise.
So, documentation is essential. But it also has a real cost. Many clinicians spend 2–3 hours a day finishing notes after sessions. That often means staying late at the office, charting at home, or catching up on weekends. The end result is less rest, less family time, and less headspace for the actual work of therapy.
Breaking Down the Core Tasks: What “Counts” as Mental Health Documentation?
Let’s translate the common documentation tasks into simple terms:
1) SOAP Notes (Subjective, Objective, Assessment, Plan)
- Subjective: What the client reports in their own words—symptoms, feelings, stressors, wins, and worries.
- Objective: What you observed—mood, affect, speech, behavior, notable physical signs, and relevant test scores or scales.
- Assessment: Your clinical judgment—diagnostic impression, risk assessment, progress toward goals, and your reasoning.
- Plan: What happens next—interventions used, homework assigned, referrals, safety plans, and the follow-up schedule.
SOAP notes are structured and thorough, which is good for care. But they can be repetitive, especially when you document similar elements for every session. That’s where time disappears.
2) ICD Coding (Picking the Right Diagnosis Codes)
- Why it matters: Insurers need a diagnosis code for billing.
- What’s hard about it: Many conditions overlap. Some symptoms fit more than one code. The “most accurate” diagnosis can change as you get more information. Picking the wrong code increases the chance of claim denials or requests for more records.
- The pressure: Every code you select carries clinical, legal, and financial implications. That’s a lot to balance at 9 p.m. after a full day of sessions.
3) Compliance (HIPAA, Audits, and Accuracy)
- HIPAA: Protects client privacy. Notes must be stored and shared securely.
- Audits: Insurers or regulators can review your records. Clear, consistent notes reduce risk and save you from scrambling later.
- Accuracy: You need to document enough to justify your decisions, but not so much that you include irrelevant or sensitive details. Finding that balance takes skill and time.
The Human Impact: Documentation Burnout
Burnout doesn’t always come from hard sessions. Often, it comes from everything that happens after: the backlog of notes, the worry about coding, the fear of audits, and the mental load of trying to remember 30 clients’ stories with precision.
Here’s what clinicians commonly report:
- Lost time: Evenings turn into charting time. Weekends become “catch-up” days.
- Mental fatigue: After a full day of listening and problem-solving, writing detailed notes requires a second wave of focus that’s hard to find.
- Reduced presence in session: When you’re worried about documentation, it’s harder to be fully present with clients.
- Cumulative stress: The system rarely pauses. The to-do list grows. That constant pressure chips away at satisfaction and well-being.
If this sounds familiar, you’re not alone—and you’re not failing. The process is simply heavy.
Where AI Helps (And Where It Doesn’t)
Artificial intelligence can’t replace your clinical judgment. It shouldn’t make diagnoses for you, and it shouldn’t write notes without your input. But AI can lighten the load by handling the repetitive parts, organizing your thoughts, and giving you a head start on high-quality documentation—while you stay firmly in control.
That’s the idea behind SOAPsync, an AI assistant purpose-built for mental health documentation. It doesn’t try to be a one-size-fits-all EHR. Instead, it focuses on doing one job extremely well: helping clinicians produce clear, compliant, and billable notes in far less time.
Meet SOAPsync: An AI Assistant Built for Mental Health Professionals
What it is: A streamlined, clinician-first tool that drafts SOAP notes from your key points, suggests diagnosis codes based on your inputs, and keeps everything within a HIPAA-aligned workflow.
What it’s not: It’s not a generic chatbot, a bulky EHR, or a replacement for your expertise. You direct it. You review its drafts. You approve the final note.
How SOAPsync Works, Step by Step
- Input your session highlights.
After a session, you enter the main points: client goals, symptoms, interventions, risks, progress, and next steps. You can also add context (e.g., “client recently lost a job,” “increased panic attacks,” “safety plan reviewed”). - Get a first-draft SOAP note in your style.
SOAPsync turns your bullet points into full sentences under Subjective, Objective, Assessment, and Plan. It uses clinical language without sounding robotic. It aims for clarity, coherence, and consistency each time. - Review and refine in minutes.
You read the draft, make edits, add nuance, or remove anything unnecessary. You stay the author. The AI is your assistant, not your voice. - See diagnosis code suggestions.
Based on your inputs, SOAPsync suggests likely ICD codes. You confirm the final choice, adjust the specifier if needed, or select a different code entirely. - Finalize and save securely.
Notes are stored with encryption inside a privacy-minded workflow. You can export, copy into your EHR, or store according to your clinic’s policies. - Watch it learn your preferences.
Over time, SOAPsync adapts to your tone and structure. If you like succinct Assessments or detailed Plans, it mirrors that style to reduce edits later.
A Before-and-After Example (Plain Language)
Without AI:
You finish a 50-minute session at 4:00 p.m. You jot a few phrases: “panic attacks 3x/week, exposure homework done 50%, GAD-7 improved, discussed sleep.” At 7:30 p.m., you sit down to turn those fragments into a full SOAP note. You hesitate on the wording. You double-check the ICD code. You finally finish at 7:50 p.m., tired.
With SOAPsync:
You enter the same key points at 4:05 p.m. SOAPsync drafts a clear, structured note in your voice. It proposes a diagnosis code based on your inputs. You edit two sentences, confirm the code, and finalize by 4:12 p.m. You leave on time.
The difference is not just speed—it’s the weight off your mind.
What About Accuracy, Safety, and Privacy?
These are the right questions to ask. Here’s how SOAPsync approaches them:
- You stay in control.
AI generates a draft. You decide what’s correct. You sign the note. - HIPAA-minded design.
Notes and identifiers are protected with encryption and secure storage. Data handling follows privacy best practices suitable for clinical records. - No “black box” diagnoses.
SOAPsync’s suggestions are exactly that—suggestions. You choose the final diagnosis code based on your clinical judgment and the client’s presentation. - Right-sized detail.
You can set preferences for how concise or detailed each section should be, helping you meet audit expectations without overexposing sensitive information.
Results Clinicians Report
Early users describe four common outcomes:
- Less time on notes (often 50–70% faster).
- Notes finished during business hours, not after dinner.
- Fewer billing headaches due to clearer documentation and better code selection.
- More clinical presence, because the admin work feels manageable.
One psychiatrist put it plainly:
“I went from finishing charts at midnight to having dinner with my family. It changed my relationship with my job.”
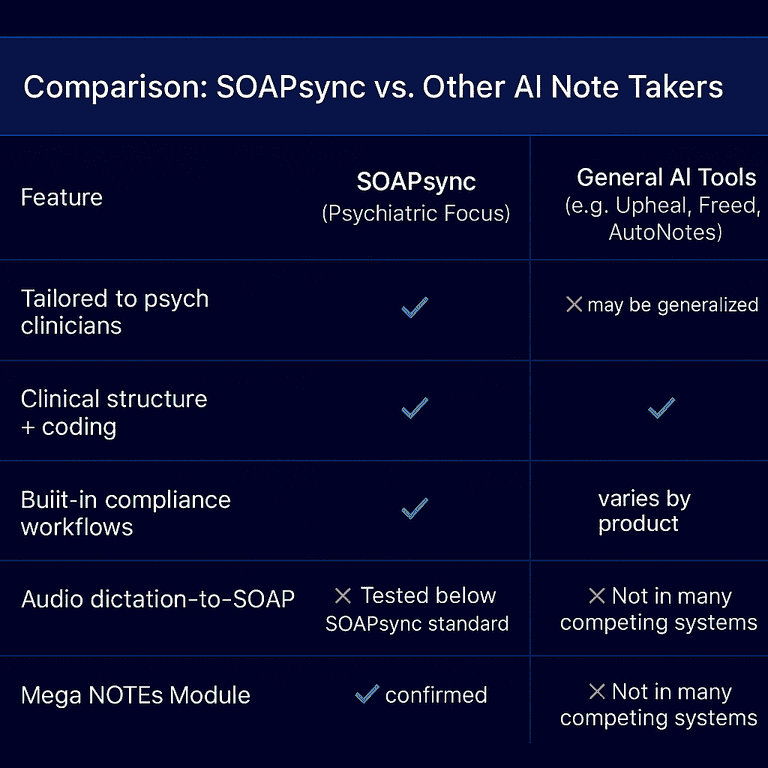
Why SOAPsync Feels Different From Typical EHRs
- Focused scope: It’s built specifically for mental health documentation. No bloated dashboards or confusing navigation.
- Clinician-first flow: The interface follows your mental model of a session, not a generic medical template.
- Low friction: You can get in, draft, edit, and finalize fast—then move on with your day.
In other words, SOAPsync doesn’t just store your notes; it reduces your cognitive load while helping you maintain your standards.
Common Questions (Straight Answers)
Will AI make my notes sound generic?
SOAPsync starts with clean, clinical language. As you edit and save, it learns your preferences—phrasing, length, and structure—so drafts feel more like you over time.
Can I still meet audit requirements?
Yes. You control what’s included. If your setting needs evidence-based interventions, measurable goals, and rationale for medical necessity, you can make those elements part of your standard template.
What if the suggested ICD code isn’t right?
You’re the clinician. You pick the final code. SOAPsync’s suggestions are there to reduce errors and speed up the process.
Will this replace my EHR?
No. Think of SOAPsync as your drafting assistant. Many clinicians export or paste final notes into their existing EHR.
Is this safe for PHI?
SOAPsync is designed with encryption and privacy practices aligned with HIPAA. You should still follow your organization’s policies for storage, retention, and access.
What about higher-risk cases?
You can tell SOAPsync to include or highlight specific safety checks (suicide risk, self-harm, harm to others, abuse concerns) and specify the actions you took. You confirm the final wording.
Practical Tips for Better Notes (With or Without AI)
- Write in session or right after. The fresher the memory, the fewer gaps.
- Use consistent headings. SOAP structure keeps you focused and makes audits easier.
- Tie Assessment to Plan. Show how your clinical reasoning led to your next steps.
- Document change over time. Reference measures, progress on goals, and any adjustments.
- Right-size detail. Include enough to justify care, but avoid unnecessary sensitive information unless clinically important.
These habits make your notes stronger. With an AI assistant, they also make your drafts faster.
Getting Started With SOAPsync
- Create your account.
- Pick a module. Choose the module you want for each SOAP note.
- Try it with a recent session. Enter highlights and review the draft.
- Customize and save. Edit and download .Done.
Most clinicians notice the time savings after a single afternoon of use.
The Bottom Line: Reclaim Your Time Without Lowering Your Standards
Mental health documentation will always be part of ethical, high-quality care. But it doesn’t need to consume your nights or your weekends. With a focused AI assistant like SOAPsync, you can get clear, complete notes done during business hours, reduce billing issues, and protect your energy for the work that truly matters—sitting with people and helping them heal.
If you’re tired of living in a chart, it’s time to try a different approach.
🎁 Free trial + $50 off your first subscription
👉 Start Saving Time Today — Click Here
Let SOAPsync handle the notes—and give you your life back.
#SOAP notes, #ICD coding for mental health, #HIPAA-compliant documentation, #therapist note-taking, #behavioral health documentation tools